Boost Practice Revenue by 23% in Just 90 Days
Struggling with denied claims, cash flow issues, or outdated billing processes?
MaxRemind delivers proven RCM strategies that increase revenue by 23%. Book a demo to learn how we streamline operations and improve financial outcomes for practices.
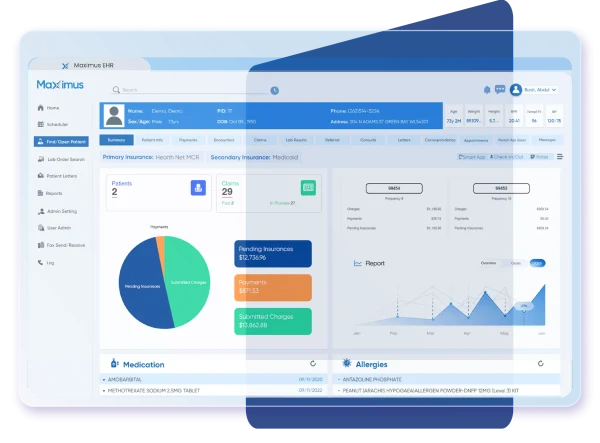








What MaxRemind RCM Offers
We simplify all your billing complexities through intelligent automation, expert oversight, and seamless operational workflows.
Scheduling & Eligibility Verification
Smooth pre-visit workflows with eligibility checks, demographics, balance info & confirmations.
Real-Time Patient Balance Updates
Immediate access to accurate patient responsibility before and after visits.
Daily & Weekly Scheduling Tools
Structured scheduling for providers, teams, and patient appointments.
Provider Re-Credentialing
Complete credentialing support for faster approvals and uninterrupted operations.
Charge Capture & Posting
Accurate charge entry powered by AI-enabled coding assistance.
A/R Analysis & Follow-Ups
Prioritizing 90+ buckets and reducing outstanding balances with diligent follow-ups.
AI-Integrated Coding Guides
Error-free coding through our RBS (Rule-Based System) for fewer denials.
Financial & Performance Reports
Daily, weekly, and monthly insights to improve decision-making.
Get paid quicker with smart billing solutions!
The Go-To Solution for Your Practice Management
MaxRemind centralizes your revenue cycle into a clean, efficient, and fully automated system from scheduling to billing. It ensures transparency and seamless operations across your practice.
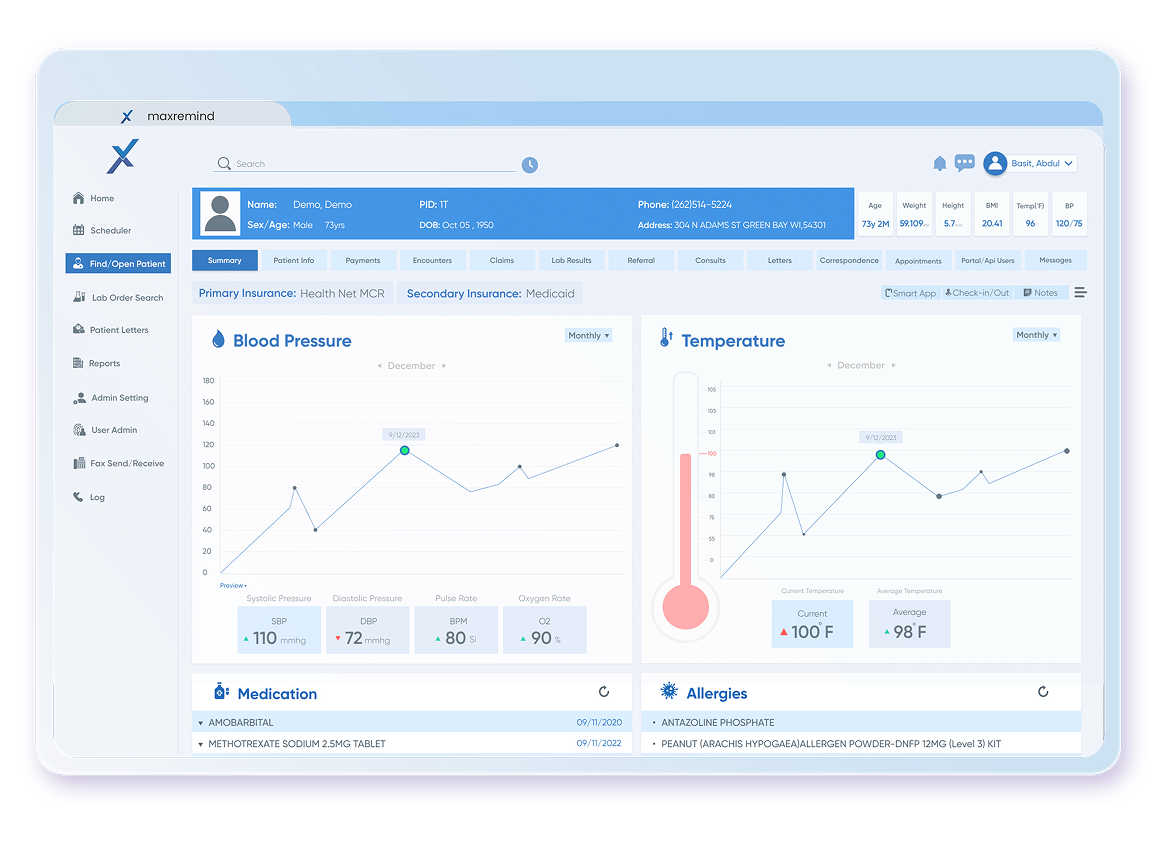
How MaxRemind Improves Your Revenue Cycle
End-to-end RCM support designed to reduce denials, accelerate payments, and maximize collections.
Appointment Scheduling
Holistic Billing
A/R Reduction
Scheduled Reporting


AI-Powered
RCM for Accurate and Faster Billing
RBS – Rule-Based System
Our RBS minimizes claim errors in the pre-submission phase, drastically reducing denials and improving revenue flow.
CDS – Clinical Decision Support
CDS enhances diagnosis, treatment planning, and coding accuracy – improving both care quality and financial performance.


Built to Deliver Measurable Financial Results
Our intelligent RCM framework focuses on revenue growth, operational efficiency, and long-term financial stability.
Streamlined administrative flows give you more time for patients.
Our billing experts guide you on capturing every charge and preventing missed reimbursements.
Quick and accurate provider enrollment for a smooth operational start.
All workflows, from appointment to payment stay synchronized and automated.
By reducing denials, improving coding accuracy, and accelerating reimbursements.
Our automated workflows eliminate manual tasks, letting you focus on patient care.
We prioritize 90+ buckets and initiate consistent follow-ups to recover outstanding balances.
Our RBS checks for coding and claim errors before submission.
Our team immediately investigates, corrects, and resubmits it – minimizing delays.
Boost Your Revenues & Save Your Time.
Keep your practice efficient, compliant, and financially strong with MaxRemind’s Healthcare RCM Solutions.
© 2026 MaxRemind Inc. All Rights Reserved.
